 
Visual acuity was 20/30-2 and improved to 20/25-2 with pinhole correction. On the first postoperative day, IOP decreased to 15 mmHg. The patient was then prescribed 250 mg acetazolamide tablets every 6 hours before he was discharged. A 250 mg acetazolamide tablet was given orally, and the IOP decreased to 30 mmHg within 1 hour. The cornea was clear, and the vault of ICL was 1.5 times of central corneal thickness (CCT). The IOP of the right eye measured with an applanation tonometer elevated to 48 mmHg. One hour after uncomplicated surgery, the patient complained of mild ocular pain. The viscoelastic agent was removed by manual irrigation with balance salt solution. The ICL was implanted in the right eye through a 2.75 mm temporal clear corneal incision. A viscoelastic agent (Alcon Laboratories, Inc., Provisc, Fort Worth, Texas, USA) was injected into the anterior chamber through a paracentesis port. Before surgery, tropicamide 1% ophthalmic solution (Novartis, Mydriacyl 1%, UK) was applied until full pupillary dilatation was achieved. The 12.6-mm ICLs were selected for both eyes. The preoperative endothelial cell counts of the right and left eyes were 27 cells/mm 2, respectively. The patient did not require preoperative preventive iridotomies because of the presence of a hole at the center of the optic part of the fourth generation of ICL. The preoperative intraocular pressures of the right and the left eyes were 17 and 16 mmHg, respectively. The white-to-white (WTW) distance measured with a caliper was 11.5 mm in both eyes. The anterior chamber depth (ACD) measured with scanning slit corneal topography (Bausch & Lomb, Orbscan II, Rochester, NY, USA) was 3.32 mm in the right eye and 3.2 mm in the left eye. His scotopic diameters of the right and left pupils measured with a corneal topography (Carl Zeiss, ATLAS TM 9000 Corneal Topographer, Jena, Germany) using PathFinder II Corneal Analysis Software were 7.0 and 6.4 mm, respectively. His pupils were reactive to light, and the diameters of pupils were equal. Preoperatively, the slit-lamp examination was completely normal. Two separate operations of ICL implantation were scheduled, starting with the right eye. Instead of undergoing laser vision correction, we recommended implantation of toric Implantable Collamer Lens (toric ICL STAAR Surgical, Nidau, Switzerland) in both eyes owing to thin corneas. The result showed that the thickness of the thinnest point of the right and left cornea was 521 and 511 μm, respectively, and no ectatic changes were detected. Corneal tomography and corneal thickness were obtained with a rotating Scheimpflug camera system for anterior segment analysis (OCULUS Optikgeräte, Pentacam, GmbH Wetzlar, Germany). He denied any past ophthalmic procedures. Compared with former reports, we noted an association between immediate control of elevation of postoperative intraocular pressure, light reactivity of the dilated pupil, and reactivity to pilocarpine 2% eye drops as potential predictors for reversibility of Urrets-Zavalia syndrome.Ī 20-year-old healthy Thai man with myopic astigmatism attended our clinic for refractive surgery. The findings of the right eye suggested diagnosis of Urrets-Zavalia syndrome. 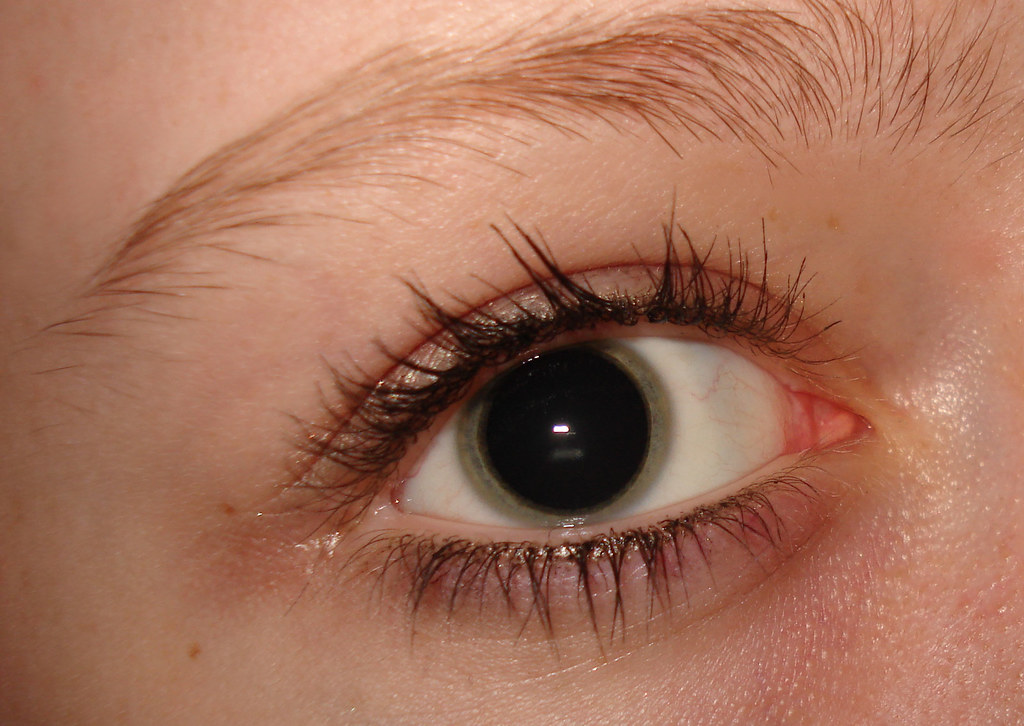
Two months after surgery, the dilatation of the right pupil partially reversed. Two weeks later, the left eye underwent the Implantable Collamer Lens implantation and showed neither postoperative increase in intraocular pressure nor postoperative pupillary dilatation. At postoperative day 1, the right pupil remained dilated but still reactive to light and pilocarpine 2% eye drops. Postoperative pupillary dilatation was detected, presumably due to effect of preoperative application of mydriatic drops. One hour after the uncomplicated surgery of the right eye, intraocular pressure increased to 48 mmHg and was immediately controlled with antiglaucoma medications. The preoperative slit-lamp examination of both eyes was normal, and no ectatic changes were detected from corneal tomography. Case presentationĪ 20-year-old Thai man with myopic astigmatism in both eyes underwent Implantable Collamer Lens implantation in the right eye. However, reversibility of pupillary dilatation is possible in some cases. Retention of the viscoelastic agent during Implantable Collamer Lens implantation can result in postoperative elevation of intraocular pressure and Urrets-Zavalia syndrome. 
Urrets-Zavalia syndrome results in complaints of glare, halo, and photophobia. Fixed dilated pupil after ophthalmic surgery or Urrets-Zavalia syndrome occurs after anterior segment surgery and usually relates to postoperative elevation of intraocular pressure. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
